Salivary gland malignancies affect 2.5 to 3 in 100,000 people each year in the United States, and comprise only 6% of head and neck cancers.1,2 Despite current imaging technologies, tumor location and heterogeneity render diagnosis and treatment decisions challenging for the treatment team. Dealing with treatment sequelae is often daunting for patients, who can face potentially devastating side effects, such as disfigurement and facial nerve paralysis.
Explore This Issue
November 2008Jesus E. Medina, MD, currently the Paul and Ruth Jonas Professor and Chairman of the Department of Otorhinolaryngology at the University of Oklahoma, has treated these patients at his tertiary referral center in Oklahoma City for more than 20 years. In that time, Dr. Medina has observed the refinement of diagnosis using superior imaging techniques in combination with fine-needle aspiration biopsy. The addition of neutron beam radiation, and facial nerve reconstruction options, have also moved the field forward. Combination treatment using surgery and radiation therapy has had a tremendous effect in our ability to give these patients a long term of tumor-free survival, he said.
 Fine-needle aspiration biopsy is very dependent on the expertise of your cytopathologist. Most people believe their needle-and this can lead to some errors in treatment. [Results of a fine-needle aspiration biopsy] are not always correct. It’s just one piece of data.
Fine-needle aspiration biopsy is very dependent on the expertise of your cytopathologist. Most people believe their needle-and this can lead to some errors in treatment. [Results of a fine-needle aspiration biopsy] are not always correct. It’s just one piece of data.-Barry M. Schaitkin, MD
Not Only Rare, but Also Diverse
At least 90% of parotid tumors are benign, but the parotid remains the most common site of malignant tumors. According to the American Cancer Society, approximately 80% of malignant salivary gland tumors originate in the parotid gland; 10% to 15% in the submandibular gland; and the remainder in the sublingual and minor salivary glands.3 Tumors in the latter tend to be malignant but are quite uncommon. As has been reported in Australian studies, the parotid is also a frequent site of metastasis from melanoma.4 Those at risk to develop salivary gland malignancies include people over the age of 50; people who received radiation treatment to the head and neck in childhood or young adulthood (such as for acne or tonsillitis); and heavy smokers (Warthin’s tumor).
The umbrella term salivary gland malignancies includes a broad spectrum of histologic tumor types. A 1999 epidemiologic study from Alabama found mucoepidermoid carcinomas to be the most frequent malignancy.5 These tumors develop most often in the parotid glands, and can vary from low- to high-grade. Adenoid cystic carcinoma (ACC) is slow-growing but persistent, leading to relatively favorable short-term prognosis but a poor prognosis beyond 10 years due to common late recurrences. ACC tumors tend to metastasize to the lungs. Most ACCs also arise in the parotid gland, and also tend to be slow-growing. Polymorphous low-grade adenocarcinomas originate most commonly in the minor salivary glands. Rare types of adenocarcinomas include basal cell adenocarcinoma, clear cell carcinoma, cystadenocarcinoma, sebaceous adenocarcinoma, oncocytic carcinoma and others. Small- and large-cell undifferentiated carcinomas are high-grade cancers that tend to spread, contributing to poor prognoses for these patients.
Thorough Diagnostics Required
Patients with salivary gland tumors often seek medical attention when they have a palpable, painless mass in either the parotid or submandibular region. Generally, most patients are not quick to come in [for diagnosis], noted Barry M. Schaitkin, MD, Professor of Otolaryngology at the University of Pittsburgh School of Medicine. Perhaps one reason for this is that the vast majority of salivary gland tumors-especially those originating in the parotid gland-are benign and slow-growing. The clinician might suspect malignancy if the patient has facial numbness; new muscle weakness on one side of the face; pain in the face, neck, or mouth; skin fixation; or enlarged lymph nodes, indicating metastasis.
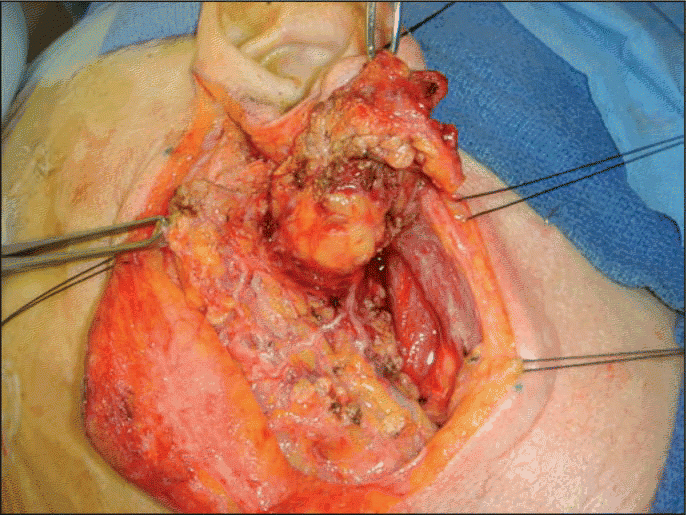
Diagnosis of salivary gland malignancy is not always straightforward, and diagnostic practices vary across regions. Following a full history and physical, as well as an imaging study (either CT or MRI), many head and neck surgeons perform tumor resection to establish a diagnosis. Some, like Dr. Medina, recommend doing a fine-needle aspiration (FNA) biopsy instead. If you have a doubt, stick a needle in it, he said. Don’t open it; don’t march in to do an open biopsy.
There is some controversy regarding the indications for FNA in the evaluation of parotid masses. Dr. Schaitkin cautioned that FNA is not 100% accurate. He recalled one 25-year-old female patient, for instance, whose aspiration biopsy was negative for malignancy, and yet he eventually removed her tumor, which turned out to be cancerous.
False positives and false negatives are not uncommon, especially when FNA is used to evaluate parotid masses. David W. Eisele, MD, is Director of the Head and Neck Cancer Program at the UCSF Helen Diller Family Comprehensive Cancer Center and Professor and Chairman of the Department of Otolaryngology-Head and Neck Surgery at the University of California, San Francisco. He and colleagues at Johns Hopkins published a review article in Current Opinion in Otolaryngology and Head and Neck Surgery in 2006 about the accuracy of fine-needle aspiration biopsy. Despite reported accuracy rates of 90% to 95%, some parotid neoplasms are prone to diagnostic error. For instance, ACC may frequently be interpreted as benign. Whether one uses the fine needle aspiration routinely or selectively in patients with parotid masses, the fine needle aspiration findings should contribute to, not displace, the overall diagnostic impression, the authors wrote.6
Fine-needle aspiration biopsy is very dependent on the expertise of your cytopathologist, asserted Dr. Schaitkin. Most people believe their needle-and this can lead to some errors in treatment. [Results of a fine-needle aspiration biopsy] are not always correct. It’s just one piece of data.
Dr. Medina emphasized that there is no substitute for a thorough preoperative evaluation, to include history, physical, and a CT or MRI scan. The 2008 National Comprehensive Cancer Network (NCCN) Practice Guidelines for Head and Neck Cancers recommend a full history and phy sical, either a CT or MRI, pathology review, chest imaging, and either FNA or open biopsy.7 A well-thought-out open biopsy is valuable, according to Dr. Medina, in selected cases where characteristics of the mass are such that an inflammatory process of metastases from elsewhere must be ruled out and the FNA is repeatedly inconclusive.
Challenges for Surgeons
Treatment for salivary gland malignancies remains primarily surgical. Adjuvant radiation is recommended to help reduce risk of locoregional recurrence if there is lymph node metastasis, a high-grade tumor, positive margins, and T3-4 stage disease.8 Definitive radiation therapy has also been used as primary treatment for salivary gland malignancies that are deemed inoperable. Dr. Eisele and colleagues from the Department of Radiation Oncology at UCSF’s Comprehensive Cancer Center found that radiation alone was effective treatment in very select patients. In their retrospective series of 45 patients treated at their center, T3-4 disease and receiving radiation doses lower than 66 Gy were independent predictors of local recurrence.9
Sources interviewed for this report emphasized that surgical intervention requires careful planning and execution. The scope of the operation may not be entirely clear preoperatively, said Dr. Eisele. For example, FNA biopsy may indicate that a parotid tumor is mostly likely malignant, but does not reveal the exact tissue type. A head and neck surgeon must be prepared, in that case, to manage the tumor intraoperatively. Important nearby structures, such as the facial nerve, may need to be sacrificed if the tumor has invaded the facial nerve or if the tumor cannot be surgically separated from the nerve. In addition, a primary nerve reconstruction, primary facial reanimation, or other reconstructive techniques may be required in an individual patient.
Surprises often develop in the OR, agreed Dr. Medina, and for that reason, he said bluntly, otolaryngologists should go in loaded for bear. In other words, If you suspect that the facial nerve may be involved, be ready and prepared to go as far as doing a mastoidectomy to expose the nerve. If you don’t do that kind of surgery routinely, have one of your otology colleagues who does this operation three or four times a week just stand by.
 If you suspect that the facial nerve may be involved, be ready and prepared to go as far as doing a mastoidectomy to expose the nerve. If you don’t do that kind of surgery routinely, have one of your otology colleagues who does this operation three or four times a week just stand by.
If you suspect that the facial nerve may be involved, be ready and prepared to go as far as doing a mastoidectomy to expose the nerve. If you don’t do that kind of surgery routinely, have one of your otology colleagues who does this operation three or four times a week just stand by.-Jesus E. Medina, MD
Treat Only at a Center?
Given the rarity of these neoplasms, the heterogeneity of tumors and cell types, and the multidisciplinary requirements of combined surgical and radiation therapy, does it make good sense for physicians to refer patients with suspected malignancies to tertiary centers? Dr. Schaitkin believes that the majority of parotidectomies can be accomplished by general otolaryngologists-head and neck surgeons. Parotid tumors are not uncommon, and many surgeons in the community do a lot of parotid tumor surgery. As long as otolaryngologists-head and neck surgeons are comfortable with their skills, they feel that they’ve adequately evaluated the patient, and it’s within their skill set, I think it’s okay.
Factors that might warrant referral to a tertiary center include large tumors, those that are suspicious for malignancy, or patients who need nerve grafts. According to Dr. Schaitkin, Surgeons should honestly assess their abilities and ask themselves, ‘Is this a patient to whom I can really offer everything they need?’ You don’t want to get yourself in the operating room and then decide that it was over your head. Doctors call me postoperatively with patients with facial paralysis and most of them wish they had not done that particular case.
Dr. Eisele believes that some patients, especially those with complex disease, are best managed using a multidisciplinary approach at a cancer center. But, he said, general otolaryngologists-head and neck surgeons are quite capable of managing parotid tumors. And in the parotid, it’s actually the exception rather than the rule that there is going to be a complex procedure requiring special expertise.
Follow-Up and New Directions
Combined surgical and radiotherapy now offers longer-term tumor-free survival rates for many patients with salivary gland cancer. However, late recurrence after five years-either local, regional, or metastatic-is not uncommon. Regular follow-up will be necessary to assess these patients for possible return of their disease.
The addition of chemotherapy to a combined regimen remains largely unverified as to efficacy; in the most recent NCCN guidelines, for instance, the panel was not in agreement about the approach of chemoradiation (using cisplatin) because there are no published studies to date for unresectable salivary gland tumors.10 Several clinical trials are currently active evaluating a number of chemotherapeutic and targeted therapies in patients with metastatic or recurrent salivary gland cancer.11 One recent phase II trial reported by the Eastern Cooperative Oncology Group showed moderate activity of paclitaxel in patients with recurrent mucoepidermoid and adenocarcinoma-type tumors. The drug produced no response in patients with adenoid cystic carcinomas.12
Dr. Eisele, who is Co-Chair of the National Cancer Institute’s Task Force on Rare Tumors, emphasizes that enrolling patients in clinical trials conducted by cooperative trial groups will furnish needed answers to questions about salivary gland malignancies. For instance, which tumor types are most likely to respond to targeted molecular therapies? Which targeted therapies already commercially available might benefit these patients?
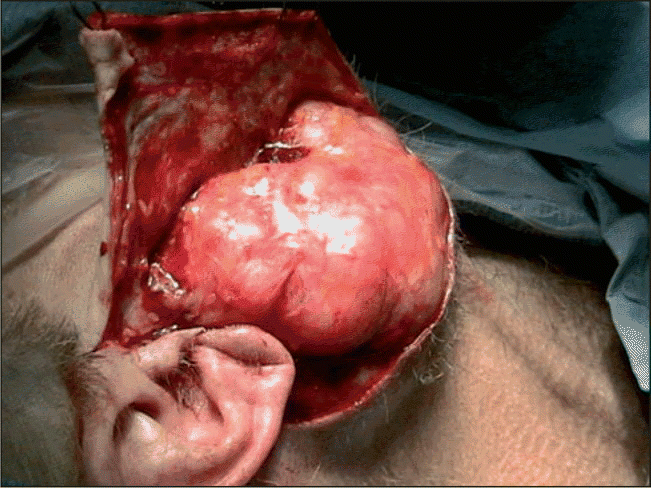
Especially for people with recurrent disease, whether it is metastatic or locoregionally recurrent, insights into the molecular underpinnings of their tumors may prove especially beneficial. Not only are these cancers heterogeneous in terms of tumor types, but the heterogeneity from patient to patient makes treatment even more challenging, he said. For instance, he observed, one patient’s adenoid cystic carcinoma might be c-Kit positive, making it a possible target for imatinib (Gleevec®). In another patient, this may not be the case. In addition to cooperative groups and the Task Force for Rare Tumors, some private foundations, such as the Adenoid Cystic Carcinoma Research Foundation (www.accrf.org ), will, he hopes, help to make strides in advancing targeted therapies.
There have also been some advances in dealing with facial paralysis. Neuromuscular retraining has been gaining recognition as an effective modality for optimal recovery from facial nerve paresis.13,14 The retraining includes the use of surface electromyographic facial nerve monitoring and sensory feedback (practicing exercises in front of a mirror) to increase activity in weak muscles, improve coordination of muscle groups, and decrease activity in hyperactive muscles. Although there are not many physical therapists specializing in nonsurgical facial nerve rehabilitation, there are some centers in the Midwest-most notably, the Neuromuscular Retraining Clinic at the University of Wisconsin Hospital and Clinics, run by H. Jacqueline Diels, OTR-to which patients can be referred. Advances in this area have the potential to immeasurably improve patients’ quality of life. A person with facial paralysis loses not just his or her self-image (which can engender social prejudice) but also the ability to convey the normal social signals of interpersonal communication. Restoring function and expression to the highest possible level results in patients’ improved health, self-esteem, acceptance by others, and quality of life.
Support for the Patient
Most patients with malignant salivary gland tumors have two major issues, said Dr. Schaitkin. Not only do these patients face a potentially life-threatening diagnosis, but the very real possibility that they will have some facial paralysis. Dr. Schaitkin, who runs a facial paralysis center, is often amazed at how close the psychosocial aspects of facial paralysis equal those of the diagnosis of cancer. Some patients with terminal prognoses still get tremendous benefit from minor facial reanimation procedures.
Physicians can help provide psychosocial support for these major issues in some of the following ways.
At diagnosis: Careful attention should be paid to conducting a candid, truthful, and gentle discussion of patients’ situations, said Dr. Medina. At his tertiary center, patients may be intimidated by initial discussions that can include up to three physicians (surgeons and radiologists) as well as trainees. Dr. Medina has found that patients at the University of Oklahoma often open up to a dedicated oncology nurse who is part of the multidisciplinary team. The multidisciplinary team at UCSF includes oncology social workers and psychologists who can provide counseling, said Dr. Eisele. This [facial paralysis as the result of surgical treatment] is a daunting thing for someone to contemplate. His team at UCSF also links newly diagnosed patients with those who have already successfully completed treatment and rehabilitation. This can be a powerful support to a patient in the early period after diagnosis and during treatment.
Suggest support: Physicians can assess their patients’ community resources-religious, social, or familial-and refer them to counseling if the situation warrants.
Pass on resources: Unguided, a patient may run into confusing and even disreputable information on the Internet, noted Dr. Medina. It is helpful to suggest credible Web sites for patients. Many associations offer online user discussion groups, where patients share information and support. Others can offer referrals to local resources. Dr. Schaitkin has co-written a book with Mark Mays, The Facial Nerve (Thieme, 2000). This is a major reference for physicians and to a lesser extent for patients with facial nerve paralysis.
Internet Resources
Supports for dealing with cancer diagnosis and treatment:
- American Cancer Society-a premier source of well-written and validated information about all types of cancer and treatments. www.cancer.org
- CancerCare-started more than 50 years ago by oncology social workers, this organization offers warm line phone consultations with trained social workers to help cancer patients with insurance, treatment and psychosocial issues. www.cancercare.org
- The National Cancer Institute offers a wealth of consumer publications about all aspects of cancer diagnosis and treatment, including Managing the Side Effects of Radiation Therapy. Many of these publications can be ordered or downloaded from the NCI publications locator Web site: www.cancer.gov/publications
Supports for dealing with facial paralysis:
- Sources of referrals to physical therapists who specialize in facial nerve retraining, as advanced by H. Jacqueline Diels, OTR, University of Wisconsin Hospital and Clinics. www.bellspalsy.ws/centers.htm
- Bell’s Palsy Information Site-although this Web site is primarily directed to those with Bell’s palsy, several excellent resources are applicable to facial nerve paralysis. Patients can click on information about the facial nerve, and facial nerve retraining. www.bellspalsy.ws
References
- American Cancer Society. What are the key statistics about salivary gland cancer? August 2006. Retrieved September 18, 2008 from www.cancer.org/docroot/CRI/content/CRI_2_4_1X_What_are_the_key_statistics_for_salivary_gland_cancer_54.asp?sitearea= .
[Context Link] - Kaszuba SM, Zafereo ME, Rosenthal DI, et al. Effect of initial treatment on disease outcome for patients with submandibular gland carcinoma. Arch Otolaryngol Head Neck Surg 2007;133:546-50.
[Context Link] - American Cancer Society. What is salivary gland cancer? August 2006. Retrieved September 18, 2008 from www.cancer.org/docroot/cri/content/cri_2_4_1x_what_is_salivary_gland_cancer_54.asp .
[Context Link] - Bron LP, Traynor SF, McNeil EB, O’Brien CJ. Primary and metastatic cancer of the parotid: comparison of clinical behavior in 232 cases. Laryngoscope 2003;113:1070-75.
[Context Link] - Pinkston JA, Cole P. Incidence rates of salivary gland tumors: results from a population-based study. Otolaryngol Head Neck Surg 1999;120:834-40.
[Context Link] - Alphs HH, Eisele DW, Westra WH. The role of fine needle aspiration in the evaluation of parotid masses. Curr Opin Otolaryngol Head Neck Surg 2006;14:62-6.
[Context Link] - National Comprehensive Cancer Network. NCCN Clinical Practice Guidelines in Oncology™; Head and Neck Cancers. Available online at www.nccn.org/professionals/physician_gls/PDF/head-and-neck.pdf .
[Context Link] - Chen AM, Granchi PJ, Garcia J, et al. Local-regional recurrence after surgery without postoperative radiation for carcinomas of the major salivary glands: implications for adjuvant therapy. Int J Radiat Oncol Biol Phys 2007;67:982-7.
[Context Link] - Chen AM, Bucci MK, Quivey JM, et al. Long-term outcome of patients treated by radiation therapy alone for salivary gland carcinomas. Int J Radiat Oncol Biol Phys 2006;66:1044-50.
[Context Link] - NCCN, see note 7.
[Context Link] - Retrieved September 26, 2008 from: http://clinicaltrials.gov/ct2/results?cond=%22Salivary+Gland+Neoplasms%22 .
[Context Link] - Gilbert J, LiY, Pinto HA, et al. Phase II trial of taxol in salivary gland malignancies (E1394): a trial of the Eastern Cooperative Oncology Group. Head Neck 2006;28: 197-204.
[Context Link] - Diels HJ, Combs D. Neuromuscular retraining for facial paralysis. Otolaryngol Clin North Am 1997;30:727-43.
[Context Link] - Cronin GW, Steenerson RL. The effectiveness of neuromuscular facial retraining combined with electromyography in facial paralysis rehabilitation. Otolaryngol Head Neck Surg 2003;128:534-38.
[Context Link]
©2008 The Triological Society
Leave a Reply