Be careful not to be too quick to say that a patient’s problems are due to canal dehiscence. A study using CT to determine the prevalence of superior and posterior semicircular canal dehiscence in a patient population in Boston calculated the prevalence of superior canal dehiscence; although the result was similar to those from previous investigations (about 9%), this study shows there is a twist-the rate of posterior canal dehiscence may be lower than previously reported.
Explore This Issue
September 2008Previously published studies were in general, large sample size populations but they did not employ sub-millimeter technique. We aren’t aware of any investigations employing sub-millimeter technique in evaluating the posterior semicircular canal, said Rohini Nadgir, MD, Assistant Professor of Radiology at the Boston University School of Medicine, who spoke at a Triological Society session at the Combined Otolaryngology Spring Meeting.
In this retrospective study, researchers reviewed CT scans from patients who had undergone temporal bone CT scans for a variety of clinical indications between July 2005 and March 2007. Scans were done using a sub-millimeter technique to evaluate the integrity of the superior and posterior semicircular canals. The scans were performed on a 64 detector row CT scanner using 0.625-mm slice thickness, in bone plus algorithm without contrast. A review was also done of 0.3-mm interval reconstructions in the coronal and sagittal planes.
The images were reviewed by two neuro-radiologists who rated the superior and posterior canals as normal, thin, or dehiscent. Clinically relevant data were reviewed by an otolaryngologic surgeon who was blinded to the interpretations of the CT. Radiographic results were correlated to the clinical findings.
Images from 454 temporal bones from 226 patients were reviewed. Of these, 19 (9%) patients were found to have dehiscence of the superior semicircular canal. Intriguingly, of these patients, none had supportive clinical evidence of the syndrome, she said. Two patients were identified as having posterior canal dehiscence, and they didn’t have clinical signs either.
Ironically, through the chart review, five patients had an initial clinical suspicion of canal dehiscence, but none had supportive radiographic evidence. The patients were found to have other explanations for their symptoms, including benign positional vertigo, endolymphatic hydrops, cholesteatoma, and otosclerosis.
Overall, the findings confirmed the same rate of superior canal dehiscence as previous studies; however, the rate of posterior canal dehiscence was much lower than published rates.
While the classic clinical presentation of Tullio’s phenomenon should always raise suspicion for the dehiscence syndrome, it is important to keep in mind that the presentation is not necessarily specific to the syndrome, she said.
Imaging studies show a higher prevalence of superior canal dehiscence than what has been found in autopsy series. This indicates that this condition can potentially be overdiagnosed if based on imaging alone. It is therefore crucial to correlate the radiographic impression with the clinical impression, she said.
Comparison of Stapedectomy Prostheses
When it comes to performing stapedectomy, the Nitinol prosthesis has several features that make it perform better than the more traditional Teflon-platinum prosthesis. It is not perfect, however, and there are some idiosyncracities the otolaryngologic surgeon needs to get used to.
According to Jason Diaz, MD, chief surgical resident at the University of Utah School of Medicine, the Nitinol prosthesis is superior in closing the postoperative air gap; however, the crimp doesn’t always go all the way around the stapes, and there are a few features that take getting used to. Dr. Diaz discussed the prostheses at the same COSM session, where he presented a study comparing the two devices.
To set the background, he described what an ideal stapes prosthesis would be like. The desired prosthesis…will not create an inflammatory reaction in the middle ear over time, he said. We also want a malleable device that can create a secure attachment to the incus, and does not cause necrosis over the long term. You also want to look for a device that has a similar mass to the stapes.
The Teflon-platinum prosthesis was originally introduced in 1956, and over the years has had some minor alterations in design. The platinum wire at the end is malleable, and the surgeon performs a manual crimp around the incus. The Nitinol device is 55% nickel and 45% titanium, with an offset shepherd’s crook that closes around the incus when it is heat-activated. This design avoids contact between the tip and the piston, increasing contact with the incus and avoiding an oval crimp, Dr. Diaz noted.
As for potential nickel allergy, we have not seen this to be a problem with the patients in our series, he said.
Study of Nitinol Prosthesis
Surgeons at the University of Utah started using the Nintinol prosthesis in select patients in 2004. Dr. Diaz presented details of a retrospective chart review of stapedectomies performed from 1996 to 2005. A total of 679 procedures were performed at the time, but for the study 419 were excluded, for various reasons including insufficient audiometric data, revision cases, treatment for conditions other than otosclerosis, or because prostheses other than the Teflon-platinum or Nitinol device were used.
A total of 260 cases (109 male, 151 female) with an age range of 15 to 77 years were included. Of these, 233 patients (90%) received the Teflon-platinum device, and 27 (10%) had the Nitinol device implanted. Generally, there was no difference in the types of otosclerotic conditions seen in the two groups, and most cases had disease around the anterior crus. In all cases, the small fenestra technique was used. A total of 91% of cases underwent stapedotomy with a laser. A drill was used in the other 9%.
Overall, the Nitinol device performed better in closure of the air-bone gap. The researchers also looked at the postoperative rate of sensorineural hearing loss, which was defined as a loss of bone conduction of 10 dB. This was rare in our study but did occur in the Teflon-platinum group (0.9%). The largest loss we noted was 17 dB, Dr. Diaz said. There were no cases of sensorineural hearing loss in the Nitinol group.
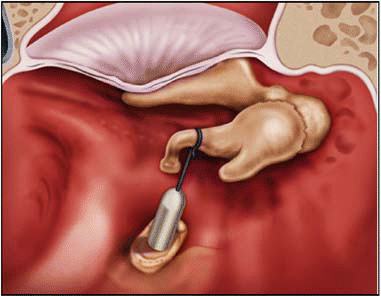
The surgeons did encounter some issues with the placement of the Nitinol device. We saw some shortening of the device when we used the laser to crimp it. We had been using a 4.25-mm Telfon-platinum device, but did note that the Nitinol prosthesis at this length came out of the oval window on several occasions. Currently a 4.75-mm Nitinol piston is most often placed, Dr. Diaz said.
Occasionally, a prosthesis bent while it was being removed from its packaging. Dr. Diaz said the problem was corrected by using a laser to straighten the shaft.
Research Continues
Since their center has been using the Nitinol device, it has undergone some minor design changes. The first-generation Nitinol prosthesis had a nice circumferential crimp; it came packaged with the shepherd’s crook around a piston. The manufacturer has changed the packaging, which no longer includes the post, Dr. Diaz said.
Researchers are continuing to evaluate the device and its performance, but so far it is staying in the lead in terms of closing the postoperative air gap.
©2008 The Triological Society
Leave a Reply