A potential solution for lack of cadaveric temoral bone has been the use of virtual or 3D-printed temporal bones to simulate the drilling exercise and provide specimens to teach anatomy and procedures.


A potential solution for lack of cadaveric temoral bone has been the use of virtual or 3D-printed temporal bones to simulate the drilling exercise and provide specimens to teach anatomy and procedures.
This four-day conference includes plenary and moderated sessions on a variety of topics on the advanced management of head and neck disease, including the nuts and bolts behind maximizing communication […]
Frailty as measured by the 5-factor mF1-5 is shown to be significantly associated with life-threatening postoperative morbidity, mortality, and length of stay following skull base surgeries.
Home drain removal is a safe and efficacious option for patients following head and neck surgery, providing cost savings to them and better utilization of providers’ time.
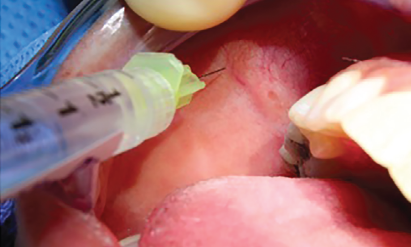
We demonstrate a novel, simplistic, and rapid approach to cannulation, dilation, and sialendoscope insertion that can be completed in an outpatient setting with the assistance of viscous lidocaine gel.
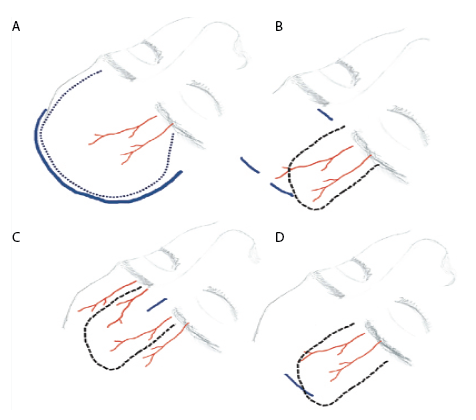
Through this endoscopic approach, glabellar incision can be avoided by performing frontal osteotomy endoscopically.

Chemoprophylaxis should be utilized in the postoperative period for vestibular schwannoma surgery.

Postoperative antibiotic prophylaxis in clean-contaminated head and neck free flap reconstruction cases is most likely sufficient and recommended for use less than 24hours from wound closure.
As technology and training standards evolve, 3D printing is emerging as a key technology in patient care in Oto-HNS.

A look at the ideal methods of skin preparation to reduce surgical site infection (SSI) in head and neck surgery.