A man with moderate dementia who is living in a nursing home is diagnosed with laryngeal cancer. The man is still able to talk and interact with other people. But he doesn’t know what year it is and is unable to make decisions on his own.



New limits on doctors in training in the United Kingdom (U.K.) have drastically reduced the amount of training they receive and may put patients in peril, a renowned retired British surgeon told listeners here on April 29 at the Annual Meeting of the Triological Society, held as part of the Combined Otolaryngology Spring Meetings.
Can supervised training with a virtual reality (VR) simulator improve performance in cadaver temporal bone dissection? Background: Cadaveric temporal bone dissection exercises are the cornerstones of otologic surgical training, but there […]
What should residency/fellowship program directors and residents making career choices know about recent trends regarding otolaryngology-head and neck surgery residents? Background: Otolaryngology, which over the years has evolved into a complex […]

Health care reform and government incentives have intensified the dialogue on electronic medical records (EMR). Despite the financial incentives for EMR adoption included in the Health Information Technology for Economic and Clinical Health (HITECH) Act, enacted as part of the American Recovery and Reinvestment Act of 2009, physician response remains lukewarm. The HITECH incentives program fails to recognize that the greatest barrier to EMR adoption is not financial, but cultural.

In an address to the 2009 Combined Otolaryngological Spring Meetings in Las Vegas, neurosurgeon Harry Van Loveren, MD, chair of the department of neurosurgery at the University of South Florida, coined the term “fogeyphobia” to describe a tendency among older doctors to become reluctant to speak out against new surgical tools and techniques, out of fear of being viewed as old-fashioned.
ACGME RRC—this litany of letters means little to most otolaryngologists. However, whether you are a private practitioner or an academician, a resident in training or a program director, you should have a basic understanding of the work done by the Accreditation Council for Graduate Medical Education Residency Review Committee (ACGME RRC).
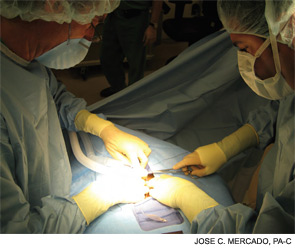
When Winston C. Vaughan, MD, told his Stanford University patients he was leaving academia to establish a private group practice, they had one question: “Are you taking Kathleen with you?” Their concern attests to the integral role that Kathleen Low, RN, NP, fills as a patient-care provider in Dr. Vaughan’s otolaryngology practice.
How do you plan to deal with workforce shortages? If you are like 55 percent of the audience at an interactive mini-seminar held during the October American Academy of Otolaryngology–Head and Neck Surgery (AAO-HNS) Foundation annual meeting, you intend to hire additional otolaryngologists to help with practice overload.

In response to many national calls to enhance patient safety, the Accreditation Council for Graduate Medical Education (ACGME) mandated a maximum 80-hour workweek for all residents beginning in 2003.