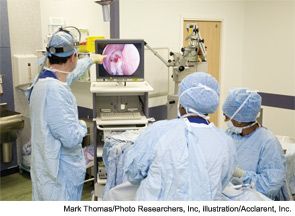
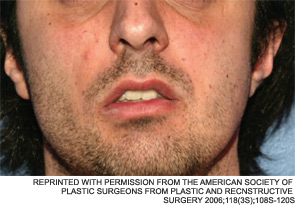
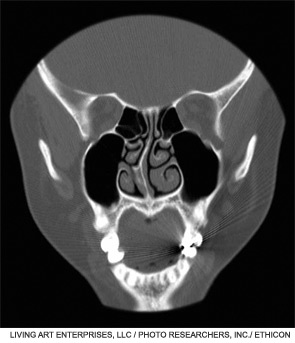
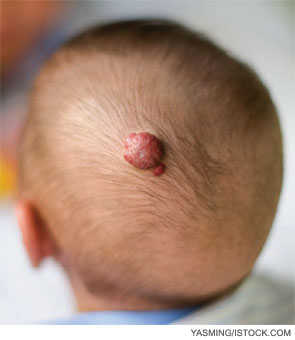
Six years after balloon sinuplasty was introduced to the otolaryngology community, it remains an evolving technology. “In my opinion, balloon dilatation has great potential, but it’s still trying to find its proper place in the ENT arena,” said Ralph Metson, MD, clinical professor of otology and laryngology at Harvard Medical School and Massachusetts Eye and Ear Infirmary in Boston.