Otolaryngologists debate recommendations on steroids, hyperbaric oxygen

For otolaryngologists seeing increasing numbers of children with sleep-disordered breathing, whether or not to refer children for a polysomnography (PSG) prior to surgery is not a decision easily made. Currently, only about 10 percent of otolaryngologists request a sleep study in children with sleep-disordered breathing prior to surgery.

Recent publication of practice parameters for surgery in adults with obstructive sleep apnea (OSA) by the American Academy of Sleep Medicine (AASM) has set off another round of debate on the need for otolaryngologists to get involved in generating their own guidelines. Although otolaryngologists have yet to agree on whether or not the time is right for guidelines on surgical treatment for sleep apnea, consensus can be claimed regarding the need perceived by the American Academy of Otolaryngology–Head and Neck Surgery (AAO-HNS) to get on the evidence-based bandwagon.

Otolaryngologists are likely to see some changes in the way informed consent is handled at the hospitals where they perform surgery. Recent changes from the Centers for Medicare and Medicaid Services (CMS), along with Joint Commission rules, have prompted many hospitals and health systems to get more involved in what previously fell firmly in the physician’s purview.

This issue of ENT Today includes an article on the debate over canal-wall-up (CWU) versus canal-wall-down (CWD) tympanomastoidectomy (p. 5). I remember hearing the same arguments when I was a resident at UCLA, which was also the last time I drilled a mastoid bone; my practice focused on head and neck surgery and pediatric otolaryngology. Over the past 32 years, Drs. Bruce Gantz, Rick Chole (two of my otology colleagues on the Board of Otolaryngology), and other otologist friends have suffered through my semi-tongue-in-cheek comments on why otologists can’t agree on which procedure is better. Although the technology used in both procedures has evolved, the final product of the two procedures, a dry, safe ear, is, as best I can tell, the same as it was when I was a resident. I have been told that one of the main factors considered in the decision regarding which procedure to perform is where the otologist trained.
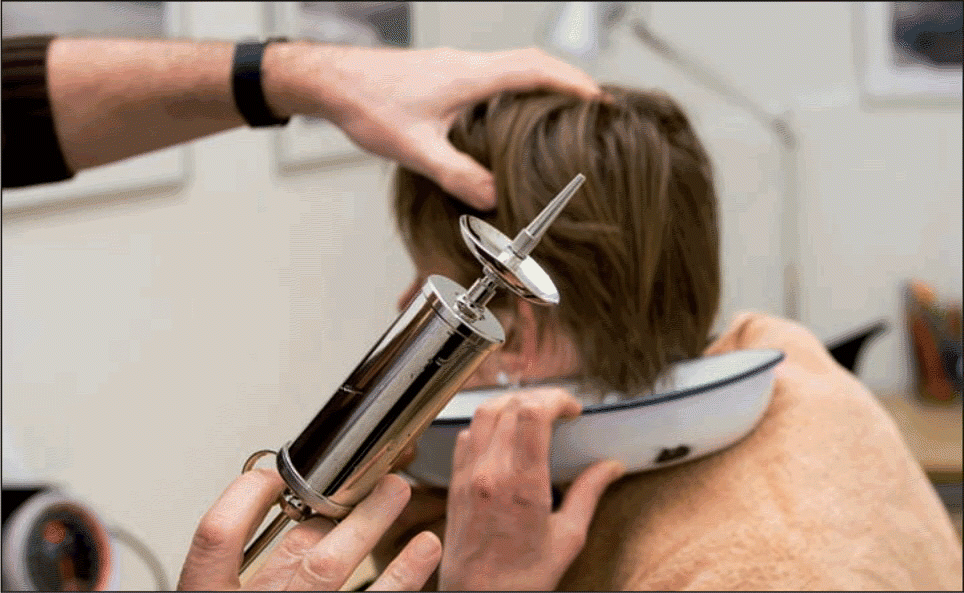
In September, the American Association of Otolaryngologists-Head and Neck Surgeons (AAO-HNS) published the first clinical practice guidelines on the removal of impacted cerumen (Otolaryngol Head Neck Surg 2008;139:S1-S21).

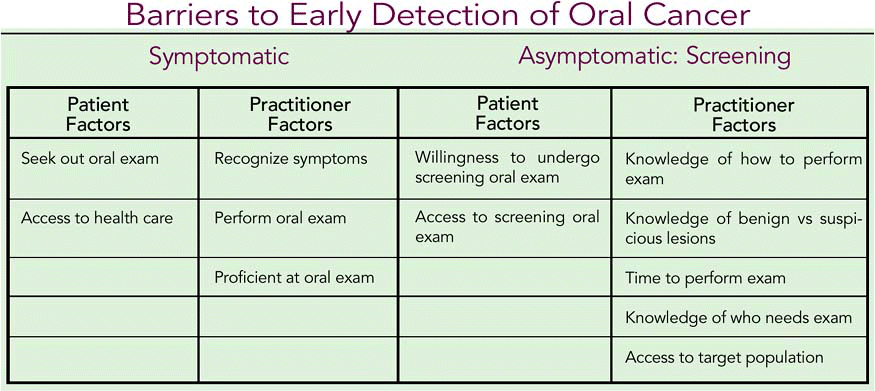
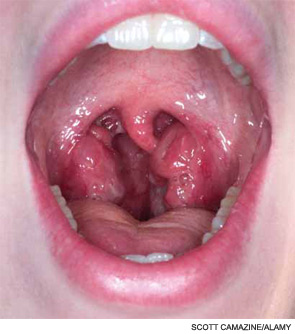
Oral screening exams are inexpensive, are easy to perform, and have the potential to reduce the annual global mortality for oral cancer by tens of thousands of people.